
Starting with Primary care quality improvement, the discussion delves into the significance of elevating quality standards in healthcare, shedding light on various strategies and challenges faced in this crucial area.
Exploring different frameworks and methodologies, the exploration of patient-centered care, preventive medicine integration, and prescription drug management reveals the intricate tapestry of improving primary care quality.
Overview of Primary Care Quality Improvement
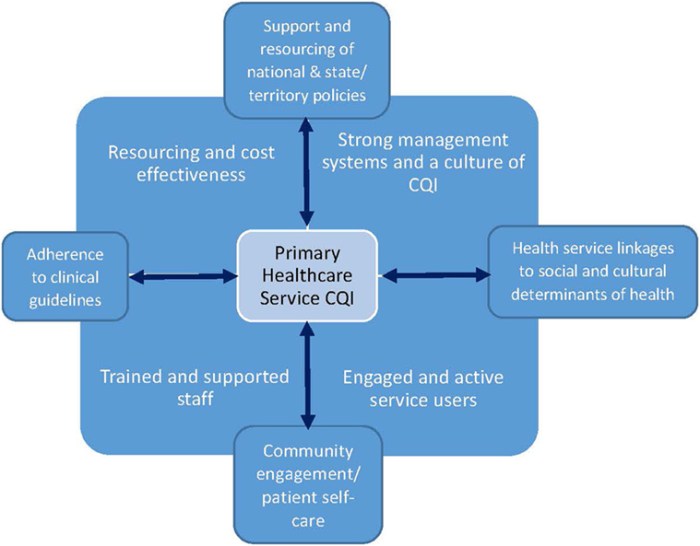
Improving quality in primary care is essential for ensuring that patients receive the best possible healthcare services. It involves focusing on enhancing the effectiveness, safety, timeliness, patient-centeredness, efficiency, and equity of care provided.
Key Initiatives and Programs
- The Patient-Centered Medical Home (PCMH) model: This model aims to improve coordination, communication, and access to care for patients by providing a team-based approach that focuses on the whole person.
- Quality Improvement Organizations (QIOs): QIOs work to improve healthcare quality at the local level by providing technical assistance, data analysis, and support to healthcare providers.
- Chronic Care Management Programs: These programs focus on managing chronic conditions efficiently and effectively to improve patient outcomes and reduce healthcare costs.
Impact on Patient Outcomes
Quality improvement in primary care has a direct impact on patient outcomes by enhancing the overall experience and effectiveness of care. Patients are more likely to receive timely and appropriate treatments, have better management of chronic conditions, and experience improved health outcomes as a result of these initiatives.
Strategies for Enhancing Primary Care Quality
Improving quality in primary care settings is crucial for ensuring better health outcomes for patients. There are various strategies that can be employed to enhance primary care quality, ranging from process improvements to the integration of technology.
Utilizing Quality Improvement Frameworks
- One common quality improvement framework used in primary care is the Plan-Do-Study-Act (PDSA) cycle, which involves planning a change, implementing it on a small scale, studying the results, and then acting on those results to make further improvements.
- Another framework is the Institute for Healthcare Improvement’s Model for Improvement, which focuses on setting specific aims, developing measures to track progress, and testing changes on a small scale before implementing them more broadly.
- Comparing these frameworks can help primary care providers determine which approach works best for their specific practice and patient population.
Role of Technology in Enhancing Primary Care Quality
- Technology plays a significant role in enhancing primary care quality by improving communication, streamlining processes, and providing better access to patient information.
- Electronic Health Records (EHRs) help in organizing patient data, tracking outcomes, and facilitating coordination among healthcare providers.
- Telemedicine and remote monitoring tools allow for virtual consultations and real-time monitoring of patients, especially useful in rural or underserved areas.
- Utilizing data analytics and Artificial Intelligence (AI) can help identify trends, predict outcomes, and personalize treatment plans for better patient care.
Measurement and Evaluation of Primary Care Quality
In order to assess primary care quality, various measures and evaluations are utilized to gauge the performance and effectiveness of healthcare services provided. This is crucial in identifying areas for improvement and ensuring that patients receive high-quality care.
Quality Indicators for Primary Care Performance
Quality indicators serve as benchmarks to measure the quality of primary care services. These indicators help in evaluating various aspects of care delivery and patient outcomes. Some examples of quality indicators used to assess primary care performance include:
- Percentage of patients receiving recommended preventive care services
- Wait times for appointments and access to care
- Patient satisfaction surveys
- Adherence to clinical guidelines and best practices
- Rate of hospital readmissions
Challenges and Opportunities in Measuring Primary Care Quality
Measuring primary care quality comes with its own set of challenges and opportunities. Some of the key challenges include:
- Difficulty in capturing the full scope of primary care services
- Variability in data collection methods and quality
- Complexity in defining and measuring outcomes
Despite these challenges, measuring primary care quality also presents opportunities for improvement and innovation. By leveraging technology, data analytics, and collaborative efforts, healthcare providers can enhance the measurement and evaluation of primary care quality to ultimately improve patient outcomes and experiences.
Patient-Centered Care in Primary Care Quality Improvement
Patient-centered care plays a crucial role in the quality improvement efforts within primary care settings. By focusing on the needs and preferences of patients, healthcare providers can deliver more personalized and effective care, ultimately leading to better health outcomes.
Importance of Patient-Centered Care
Patient-centered care ensures that healthcare services are tailored to meet the individual needs of each patient, taking into account their unique circumstances, values, and preferences. This approach not only improves patient satisfaction but also enhances the overall quality of care by promoting better communication, shared decision-making, and improved treatment adherence.
- Empowers patients to actively participate in their own care
- Builds trust and strengthens the provider-patient relationship
- Leads to more accurate diagnoses and appropriate treatment plans
Utilization of Patient Feedback
Patient feedback is a valuable source of information that can be used to identify areas for improvement within primary care practices. By listening to patient experiences, concerns, and suggestions, healthcare providers can make informed changes to enhance the quality of care they deliver.
- Conducting patient surveys to gather feedback on their experiences
- Implementing suggestion boxes or online portals for patients to share their thoughts
- Reviewing patient complaints and addressing any recurring issues
Impact of Patient Engagement
Patient engagement has a significant impact on improving primary care quality by promoting better health outcomes, increased patient satisfaction, and enhanced care coordination. When patients are actively involved in their care and feel heard and respected, they are more likely to adhere to treatment plans, follow up on appointments, and take ownership of their health.
- Reduces medical errors and enhances patient safety
- Improves treatment outcomes and overall healthcare experience
- Empowers patients to make informed decisions about their health
Integration of Preventive Medicine in Primary Care Quality Improvement
Preventive medicine plays a crucial role in enhancing the quality of primary care by focusing on proactive measures to prevent diseases and promote overall health and well-being.
Benefits of Preventive Medicine in Primary Care
- Preventive medicine practices help identify risk factors early on, allowing healthcare providers to intervene and prevent the development of chronic conditions.
- By promoting healthy lifestyle behaviors and routine screenings, preventive medicine contributes to early detection of diseases, leading to better outcomes and lower healthcare costs.
- Emphasizing preventive care in primary care settings fosters a culture of wellness and patient education, empowering individuals to take charge of their health.
Examples of Preventive Medicine Interventions
- Immunizations: Administering vaccines to prevent infectious diseases such as influenza, measles, and HPV.
- Screenings: Conducting regular screenings for hypertension, cholesterol levels, and cancer to detect issues early.
- Lifestyle Counseling: Providing guidance on healthy diet, exercise, and smoking cessation to reduce the risk of chronic conditions.
- Health Education: Offering information on preventive measures and self-care practices for maintaining optimal health.
Addressing Prescription Drug Management in Primary Care Quality Improvement
Prescription drug management is a critical aspect of primary care quality improvement, as it directly impacts patient outcomes and overall healthcare effectiveness. Challenges associated with prescription drug management in primary care include medication errors, adverse drug reactions, non-adherence to prescribed regimens, and drug interactions. These challenges can result in compromised patient safety, suboptimal treatment outcomes, and increased healthcare costs.
Optimizing Prescription Drug Use
- Implementing electronic prescribing systems to reduce errors and streamline medication management.
- Providing comprehensive medication counseling to patients to ensure proper understanding of prescribed medications.
- Utilizing medication therapy management services to optimize drug therapy and improve patient adherence.
- Engaging in regular medication reviews and assessments to identify and address potential issues promptly.
Importance of Medication Reconciliation
Medication reconciliation is a crucial component of primary care quality improvement efforts as it involves creating a complete and accurate list of a patient’s current medications and comparing it to the physician’s orders. This process helps to prevent medication errors, duplication, and omissions, ensuring safe and effective treatment for patients. By reconciling medications during transitions of care or clinical encounters, healthcare providers can enhance patient safety and reduce the risk of adverse drug events.
Public Health Initiatives and Primary Care Quality Improvement

Public health initiatives play a crucial role in supporting and enhancing quality improvement efforts in primary care. By collaborating with public health agencies, primary care providers can leverage resources, expertise, and data to improve patient outcomes and population health.
Intersection between Public Health Initiatives and Primary Care Quality Improvement
Public health initiatives focus on preventing diseases and promoting health at a population level, while primary care quality improvement aims to enhance the delivery of healthcare services at the individual level. By aligning these two approaches, healthcare systems can achieve better health outcomes for both individuals and communities.
- Public health programs often provide valuable data and insights into population health trends, which can inform quality improvement initiatives in primary care settings.
- Collaboration between public health agencies and primary care providers can lead to the development of targeted interventions and strategies to address prevalent health issues within specific populations.
- By integrating public health best practices into primary care quality improvement efforts, healthcare systems can deliver more effective and efficient care to patients.
Successful Collaborations between Public Health Agencies and Primary Care Providers
Public health agencies and primary care providers have successfully collaborated on various initiatives to improve healthcare delivery and outcomes. Some examples include:
- Joint programs to address chronic disease management and prevention, such as diabetes management clinics or smoking cessation programs.
- Collaborative efforts to promote immunization and vaccination campaigns within communities to prevent the spread of infectious diseases.
- Data-sharing partnerships to track population health indicators and measure the impact of quality improvement initiatives on overall health outcomes.
In conclusion, Primary care quality improvement is not just a concept but a dynamic process that continuously evolves to meet the ever-changing needs of patients and healthcare systems. Emphasizing patient engagement, technological advancements, and collaborative efforts, the journey towards enhanced primary care quality is a collective endeavor that shapes the future of healthcare.
Question & Answer Hub
How is primary care quality measured?
Primary care quality is measured through various indicators such as patient satisfaction surveys, clinical outcomes, and adherence to best practices.
What role does technology play in enhancing primary care quality?
Technology aids in streamlining processes, improving communication, and facilitating data analysis to identify areas for quality improvement within primary care settings.
Why is patient-centered care important in quality improvement efforts?
Patient-centered care ensures that healthcare decisions are made in partnership with patients, leading to better outcomes, increased satisfaction, and improved overall quality of care.





